Christian-History.org does not receive any personally identifiable information from the search bar below.
Graft Versus Host Disease
Graft versus Host Disease is unique to those who have had their immune system replaced through a bone marrow or stem cell transplant.
Ad:
Our books consistently maintain 4-star and better ratings despite the occasional 1- and 2-star ratings from people angry because we have no respect for sacred cows.
Disclaimer and Introduction
I am not a scientist or doctor. I am a bone marrow/stem cell transplant recipient who has Graft vs. Host Disease. At the end of this page I will refer you to reliable scientific and hospital pages that can give medical advice.
I am writing this page because a discussion by a patient has value and adds interest and personality to the subject. As far as I know, everything I say on this page is accurate and covered pretty well, but you should see a doctor before embarking on any of your own treatment!
I personally am under the supervision and care of the incredible Stem Cell Transplant team at Vanderbilt Medical Center in Nashville, Tn. My thanks to the Hematology Oncology team as well, who saved my life, put me in remission, and got me to the transplant unit.
When a person receives a transplant of an organ, such as a kidney or liver, one of the major worries is rejection. Will the patient's immune system reject the new kidney or liver. If so, the transplant will be a failure.
When bone marrow is transplanted, however, the entire blood system is replaced because it is our bone marrow that makes our blood. Along with the blood system, our immune system is replaced. Thus, we do not have to worry about our immune system rejecting the transplant because our immune system is destroyed prior to the transplant. (This is too general, but I will explain more below.)
Bone marrow transplants are performed for leukemia, lymphoma, multiple myeloma, and other blood cancer patients, although I am told that partial transplants are sometimes performed to help prevent rejection in organ transplant cases.
The danger for a bone marrow transplant (BMT) recipient is that the new immune system will attack any or all organs in our bodies because every one of our organs is foreign to the immune system.
That attack, by a transplanted immune system, is called Graft Versus Host Disease.
Doctors do their best to match the donor to the recipient. They check certain sections of both persons' DNA, genes known as HLA genes. HLA genes are the ones that control our immune system. Despite as much care as possible, it is uncommon for BMT recipients to completely avoid Graft versus Host Disease (GVH). About 80% of patients suffer, temporarily or permanently, from GVH, and about 20% of those who do die from it. Doctors take GVH very seriously.
Now that you know what Graft versus Host is, let's give you a brief overview of bone marrow/stem cell transplants so that we can understand specific symptoms and treatments.
Bone Marrow/Stem Cell Transplant
There are several ways of replacing a person's bone marrow, but all of them involve the amazing process of simply introducing the donor's bone marrow or stem cells from the bone marrow into the patient's blood stream. Nature takes over from there!
The Patient
The patient is prepared for transplant either by completely destroying (myeloablative) or partially destroying (non-myeloablative or "reduced intensity") their bone marrow. This is done by chemotherapy and sometimes radiation.
Non-myeloablative preparatory regimens are normally used for older patients, especially over 70, or those that have some other sort of health problems. A few years ago, it was uncommon to attempt a full intensity transplant on persons over 60 years old, but as technology progresses, this is becoming more common.
The Donor
The donor is prepared for donation by being given a growth hormone to stir bone marrow production. If a lot of growth hormone is given to the patient, the bone marrow will push "hematopoietic" or blood-related stem cells into the blood stream, and those stem cells can be harvested by a machine similar to kidney dialysis.
If a little hormone is given, then a doctor or nurse practitioner draws out a large amount of bone marrow by making hundreds of needle-sized holes in the donor's hip bone. The donor is anesthetized during the process, and those who have experienced it report that they feel like they've been kicked in the rear end by a mule. The soreness lasts one to two weeks.
A donor who gives stem cells can possibly fare better. Such a donor has to sit through a long 4-5 hour filtration process, but usually the soreness is less. There is soreness because the high doses of growth hormone stresses the bones and produces something similar to "growing pains."
A friend of mine who donated stem cells to his brother went through a bit more than growing pains. He had trouble sleeping for four or five days before the transplant. Usually, once the extra cells are extracted from the blood stream, there is relief, but my friend was sore for two or three days afterward.
Cord Blood: Infant Stem Cells
I, on the other hand, received my stem cells from a donated umbilical cord and placenta. The doctors were unable to find a suitably matched donor for me, and my brothers and sister were almost no match at all!
I should say that I received my stem cells from <em>two</em> donated umbilical cords because I did. One was a boy, and one was a girl. In that case, the doctors extract as much blood from the placenta and cord as possible, then, again, simply inject it in the patient—in this case, me. I got 11 or 13 (can't remember which) very large hypodermic needles worth of placenta blood pushed into my IV line. You can see it below. Yeah, we filmed it.
Note that cord blood donations are made from normal births, not abortions. The umbilical cord is always cut off a baby in a live birth, and the placenta is often discarded. In the modern age, though, those placentas and cords are lifesavers!
Autologous Transplants
There is also the situation where a patient is also the donor. In cases where relapse of the original bone marrow cancer seems unlikely, a bone marrow transplant can be made from the patient to himself or herself.
The patient is put into remission by chemotherapy. The way this works is that the chemotherapy destroys the bone marrow and, hopefully, all the cancer with it. A somewhat thorough chemotherapy is done on the patient, and then the hospital waits for the bone marrow to grow back. Once it does, they take bone marrow from the patient, or stem cells, and they store it. The doctors then run through at least one and probably two or three more "consolidation rounds," which are easier than the original "induction round" meant to put the patient in remission from his blood cancer.
After all this, a thorough destruction of the bone marrow is performed, and the patients extracted marrow cells are given back to him as transplant.
The benefit of an autologous transplant is that there is no risk of Graft versus Host. It is the patient's own immune system that is regrowing.
I have a whole page on bone marrow and stem cell transplants if you want more details.
Likelihood of Graft Versus Host Disease
I explained the types of bone marrow transplant because they produce a different risk of GVH.
Adult donors are supposed to produce a higher rate of Graft versus Host Disease. Because the use of cord blood for stem cell transplants is somewhat new, the occurrence of GVHD in cord blood recipients is not nailed down. I have heard the figure 50% thrown around.
It is more like 80% for adult donor recipients.
In my case, GVH set in within three weeks of my transplant. It takes that long, or close to that long, for the new bone marrow to "engraft," or to get from the blood stream to the bones of the torso, hips, and thigh and begin producing new blood.
Recipients of adult marrow or cells typically engraft a week faster than cord blood transplant recipients like myself, often seeing blood counts begin to rise in 10 to 14 days.
Oddly enough, I experience Graft versus Host Disease before my blood counts started rising. Normally, you need at least a few white blood cells to experience GVH, since your white blood cells are your immune system. Apparently, though, mine went to work on my skin and stomach before they even became prolific in my blood stream.
Types of Graft Versus Host Disease
I don't think it's technically accurate to describe GVH as having "types." Nonetheless, symptoms tend to cluster in three categories:
- GVH of the skin
- GVH of the gut
- GVH of the eyes
- GVH of the lungs
- Advanced GVH
- Acute vs. Chronic GVH
GVH of the Skin
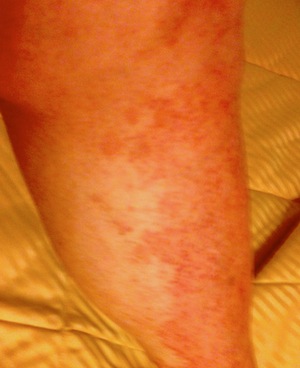 This is my lower leg. My GVH rash was extensive, but not as severe as some people get.
This is my lower leg. My GVH rash was extensive, but not as severe as some people get.GVH of the skin involves rashes and even a drying and hardening of the skin that can be debilitating. I have only had rashes, which have not been painful, nor have they even been itchy.
I have had both smooth and bumpy red patches over large amounts of my skin. At its worst it has covered all my lower leg, about half of each thigh, over half of my torso, and large parts of my torso and forearms. I have seen pictures of others, though, who have had large brown, leathery, hard sections across their rib cage and back. Such problems can hit any body area and prevent normal movement, especially if it crosses a joint.
GVH of the Gut
Graft-vs-Host of the gut covers more than just the stomach. To the medical profession, your gut runs from your lips to your anus. Thus, GVH of the gut can include mouth sores and hemorrhoids as well as indigestion, nausea, diarrhea, and vomiting. The mouth sores can make their way into the esophagus and throat as well, becoming intensely painful.
Part of the treatment for Graft versus Host Disease is immune suppression. Doctors provide medications that suppress the immune system. That means that transplant recipients suffering from GVH are more vulnerable to sickness and infections. Mouth sores and especially esophagus sores can thus be life-threatening to the patient.
GVH of the Eyes
I'll describe this one from personal experience. GVH of the eyes is very common among transplant recipients, and it varies widely in intensity.
The first time I experienced it, I was climbing into my car in a grocery store parking lot. As I turned and sat in the driver's seat, the sun caught my eyes right under the rear-view mirror of the car. I felt a stabbing pain in my left eye, and I flinched back immediately.
My eye began to water extensively, so much that I was sniffling and blowing my nose. Every time I opened my eye, it stung like someone was pouring chlorine into it. It took over 15 minutes before my eye stopped watering enough for me to drive, and the pain didn't go away for over two hours. Ouch!
It got worse from there. Soon I couldn't watch a movie all the way through. I needed sunglasses all day long, even on cloudy days, and even indoors. In fact, I did me best to wear wraparound sunglasses because wind was a culprit as well.
It was unpredictable. I could be sitting in my living room, and a lamp that had been on for an hour would suddenly catch the corner of my eye and initiate what I began to call an "eye attack."
The funny thing was that removing the irritant that caused the problem was no solution. Once my immune system had begun a GVH attack, I had to get my immune system to stop, not the irritant to stop. That involved painfully waiting with my eyes close, sometimes for two hours.
I did find an unusual remedy for the eye attacks that has been working for me for at least a couple months now. (That link is not an ad. I'm not selling anything. It links to my blog where I explain a simple method of pressing on your eye that may or may not work for you. I got it from instructions on one of my eyedrops. Works great for me, so I'm sharing it.)
GVH of the Lungs
I don't know as much about this because I haven't had any. I do know that the doctors treat me prophylactically (on a preventative basis) for pneumonia, and they strongly push exercise.
Graft versus Host of the lungs can produce shortness of breath and scarring of the lung tissue. Obviously, it is no minor problem.
I'm afraid I do not know how GVH of the lungs is treated except by general immunosuppression, which is true for all types of GVH.
Advanced GVH
This is not a real "type" of GVH. None of the others were, either, because Graft versus Host Disease is a general term for the transplanted immune system attacking any body part.
Still, we transplant recipients and our doctors talk about GVH of the skin, gut, eyes, and lungs. We don't talk about "advanced Graft versus Host" in those words.
We do, however, worry about GVH advancing, and we live in a constant battle to keep the disease in check.
For example, my doctors tell me that the more advanced my GVH of the skin gets, the more rapidly it will spread. Once it spreads over 50% or more of my body, then there is danger of my immune system moving on to my kidneys, liver, or spleen, where the danger multiplies. It is at that level that patients begin to die.
GVH of the eye is not normally associated with this kind of advance. GVH of the eyes has its own dangers: blindness or long term vision problems. In fact, in some patients, the lining of the eyelids dry so much that the lower or upper eyelids can curl in so that the eyelashes poke into the cornea.
GVH of the skin and gut, though, have to be kept at bay so that they don't progress to vital organs.
Acute vs. Chronic GVH
All the literature I've read on Graft versus Host—and lots of such literature is given to a bone marrow transplant patient—references the difference between acute and chronic GVH. Times are changing, though.
Acute GVH is the initial onset of Graft versus Host. Apparently, it is usually more aggressive and more dangerous. Chronic GVH, which has a later onset, usually longer than 100 days after transplant, is less agressive and easier to control.
Doctors are not abandoning the difference between acute and chronic GVH, but they are letting go of the time frames. Dr. Jagasia, who heads up Vanderbilt Medical Center's Stem Cell Transplant team, told me that my GVH of the skin is acute, not chronic, even though it's been well over a year since my transplant.
When I mentioned this to a doctor that was speaking at a bone marrow transplant conference in California, the doctor told me that my doctor must be up on the latest research. Acute GVH should be distinguished by symptoms, not by time frame.
Treatment of Graft Versus Host Disease
GVH, except sometimes GVH of the eyes, is always treated with immunosuppression. Currently, I am taking 1 milligram of a drug called Tacrolimus, and 20 milligrams of a steroid called Prednisone. Both of those suppress the immune system, helping my skin, eyes, and gut to stand a chance against those immune system attacks which we call Graft versus Host Disease.
In addition to immunosuppression, I have been given a steroid cream that I rub over my entire body 2-3 times a day. Currently, almost 18 months after my transplant, I am rash-free. That has not been true since less than 3 weeks after transplant. It has only been true for less than two weeks.
We are trying to taper, or slowly wean off, those immunosuppressives, but we have to carefully monitor whether the rash returns or whether there any other GVH flares up. I am having some indigestion, and immense amounts of stomach growling, burping, and gas on some days as we reduce my immunosuppressive doses.
For my eyes, I have been prescribed a drug called Restasis. I take it as an eye drop. My eye doctor says that it is the only thing known that can increase tear production.
My tear production is 50% of normal in my right eye, and 30% of normal in my left eye. I know of someone in Hawaii who has no tear production in either eye due to Graft versus Host.
The doctor also prescribed me a steroid eye drop for the "eye attacks."
Interestingly enough, the steroid drop calls for me to press in the inner corners of my eyes for two minutes after putting the drop in. I started doing this without the drop, and I realized I didn't need it. Pressing on the inner corner of my eyes stops an eye attack within a couple minutes! I was thrilled. Now I do a version of that several times a day, laying the rest of my finger across my eyelashes, where there are oil glands to coat the eye. The result is that I have been able to get rid of the sunglasses, watch movies, and work on the computer all day long with minimal eye irritation.
I do not know why that works, but it does.
Finally, I have not been given anything other than standard pharmaceuticals for GVH of the gut. I've had enough hemorrhoids on an ongoing basis to have become an expert on how to prevent and treat those in myself. For my stomach, however, the doctor has recommended such basic, off-the-shelf medications as Prilosec and Tums.
I also try natural medicines. I take a probiotic, which is bacteria that is good for your stomach and can be bought anywhere you can buy vitamins. I take fish oil in hope that my intestines won't be so dry. I eat things like ginger, for the sake of keeping my stomach settled.
Conclusion
I hope that has been an interesting and thorough look at Graft versus Host Disease. I am sure that you will understand it better having read what's above.
You can find more authoritative information on GVH and all its types from your oncologist primarily, but research can be found at sites like:
You can search published scientific research on Graft versus Host at PubMed.
Don't forget to check out the page I wrote on Bone Marrow Transplants, and especially don't miss the thrilling story of what I call a precious gift from God, my dance with leukemia that I call Yippee! I Have Leukemia.
Early Church History Newsletter
You will be notified of new articles, and I send teachings based on the pre-Nicene fathers intermittently.
When you sign up for my newsletter, your email address will not be shared. We will only use it to send you the newsletter.
